The MHA recently updated its analysis of Medicaid and Medicare enrollment based on February 2026 data. The analysis includes program enrollment as a percentage of each county’s total population and the split between fee-for-service and managed care organization. Just over 25% of Michigan’s total population is enrolled in Medicaid and 23% is enrolled in Medicare.
Roughly two-thirds of Michigan’s 2.5 million Medicaid beneficiaries are enrolled in one of nine managed care plans.
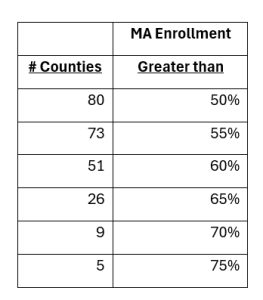
Total Medicare enrollment is 2.3 million with 64% of beneficiaries enrolled in a Medicaid Advantage (MA) plan with only three counties having less than 50% of total Medicare enrollment in MA plans. MA enrollment by county ranges from 44% to 79%, with 73 counties having 55% or more of their Medicare population enrolled in an MA plan as highlighted below.
February enrollment is spread across 45 MA plans with up to 29 plans covering beneficiaries in several Michigan counties, with a minimum of five plans available in each county.
Members with enrollment questions should contact the MHA health finance team.